The article has been reviewed by Dr. Lee Yin Yin, Candice, Specialist in Respiratory Medicine, St. Paul's Hospital
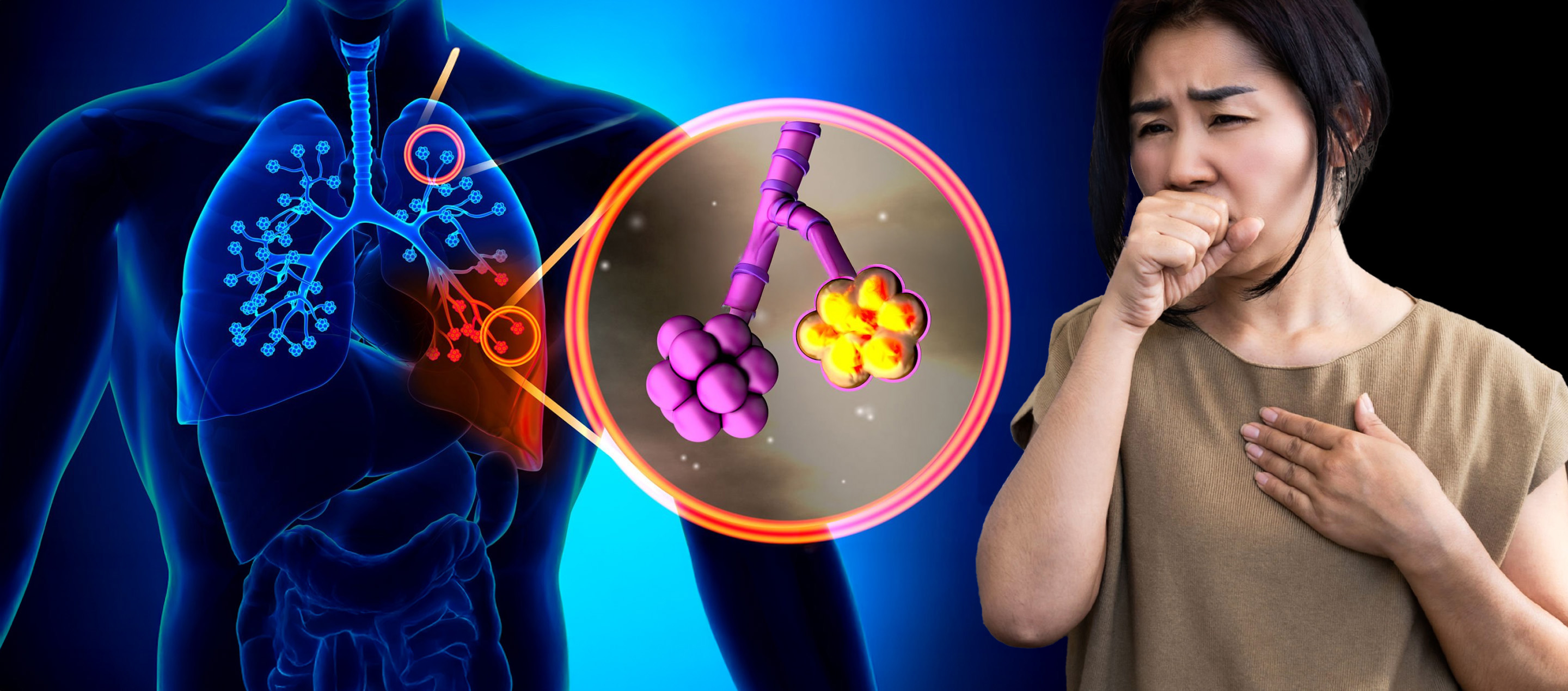

Pneumonia is a common yet potentially serious respiratory disease characterized by an infection and inflammation of lung tissue. When the lung alveoli accumulate fluid or pus, it hampers gas exchange, leading to typical pneumonia symptoms like cough, fever, and difficulty breathing. This not only severely affects respiratory function, but if treatment is delayed, it can quickly worsen and lead to multiple organ failure. This article will provide comprehensive information to help you understand the causes of pneumonia, recognize its various signs, and grasp the latest treatment and prevention methods for early intervention and management.
( ![]() Click the image to enlarge )
Click the image to enlarge )
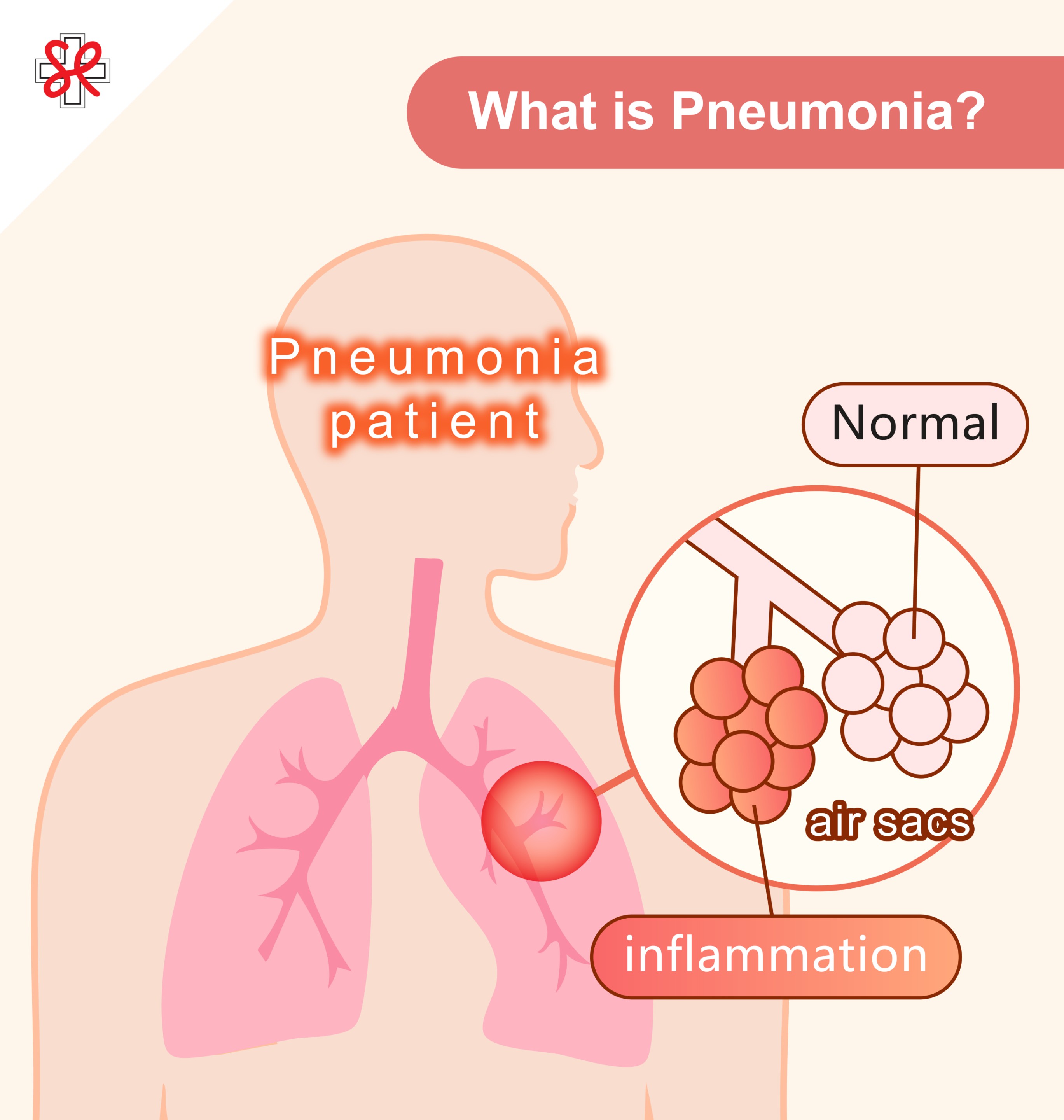
What is Pneumonia?
Pneumonia refers to the inflammation of the alveoli (air sacs) at the end of the lungs and surrounding tissue. Healthy alveoli primarily function to transport oxygen into the blood and remove carbon dioxide. However, when these alveoli become inflamed due to the invasion of bacteria, viruses, or other pathogens, they can accumulate fluid or pus (purulence), obstructing gas exchange and causing difficulty in breathing. Pneumonia can affect one or both sides of the lungs and, without timely and appropriate treatment, may evolve into life-threatening complications such as multiple organ failure.
Main Causes of Pneumonia
The causes of pneumonia are diverse and mainly arise from pathogen invasion of the lungs.
Bacterial Pneumonia
Bacteria are the most common cause of pneumonia in adults.
- Typical Pneumonia: Mainly caused by Streptococcus pneumoniae, it usually has a sudden onset with prominent symptoms.
- Atypical Pneumonia: Caused by atypical pathogens, such as Mycoplasma pneumoniae, Chlamydia, or Legionella. Symptoms of this type of pneumonia tend to be milder and have a slower onset.
Viral Pneumonia
Common viruses include influenza virus, respiratory syncytial virus (RSV), and the recently concerning novel coronavirus (COVID-19). The risk is particularly higher for older adults and immunocompromised individuals (such as children) during winter epidemics. Early symptoms of viral pneumonia may resemble those of influenza but can worsen and lead to respiratory failure.
Aspiration Pneumonia (Aspiration Pneumonia)
This occurs when a patient accidentally inhales foreign materials such as food particles, stomach acid, or saliva into the lungs, which can cause infection from the foreign material or bacteria in the mouth. This type of pneumonia is more common in individuals with compromised swallowing function (e.g., post-stroke), reduced consciousness, or bedridden elderly patients.
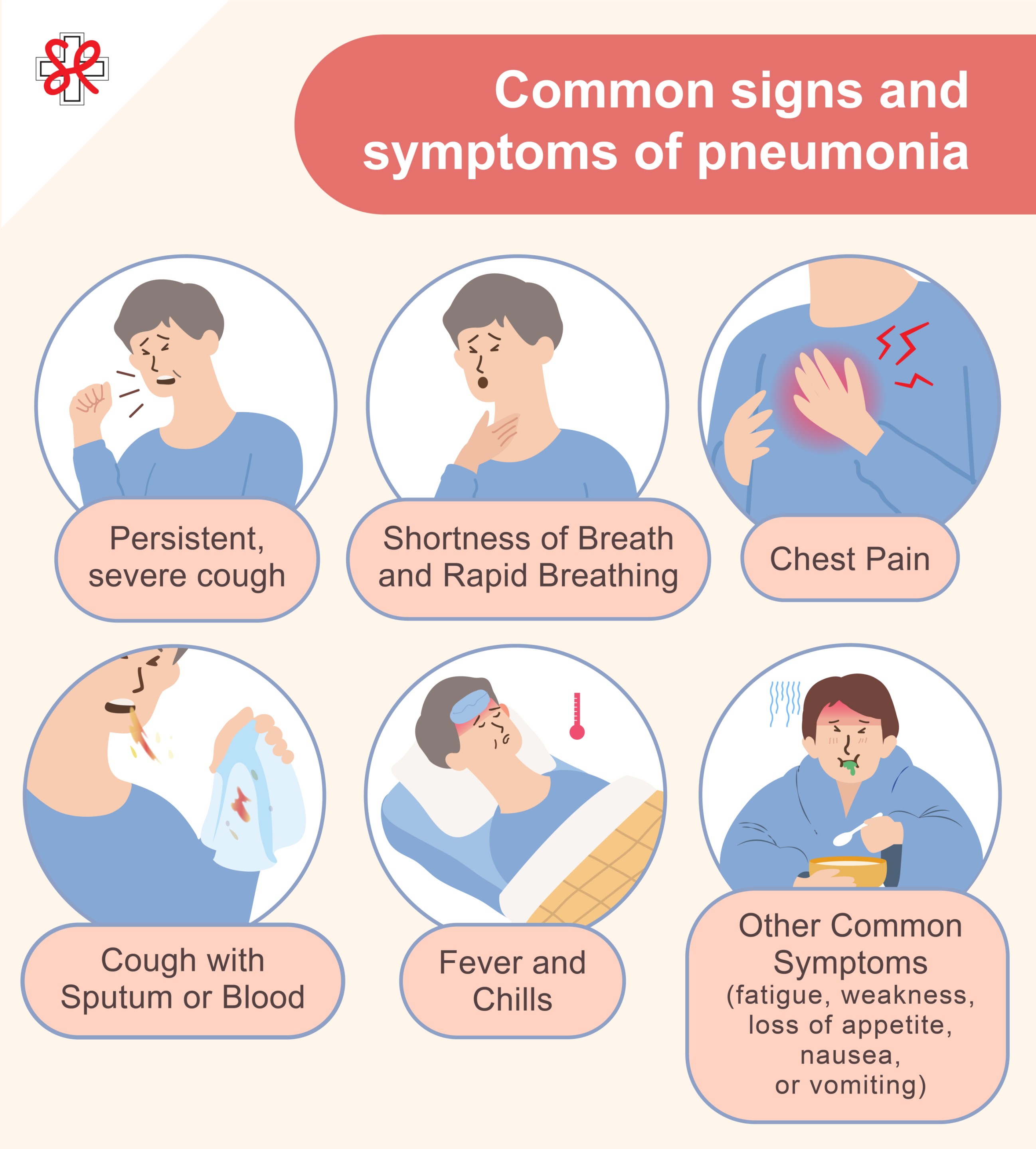
Common signs and symptoms of pneumonia
The severity of pneumonia symptoms varies depending on the type of infection, the patient's age and overall health.
( ![]() Click the image to enlarge )
Click the image to enlarge )
Persistent, severe cough
This is one of the most common symptoms of pneumonia. The cough may persist for several weeks and can be difficult to relieve.
There are mainly two types of cough associated with pneumonia:
- Productive Cough (Wet Cough): This type of cough often comes with mucus, which may be purulent or yellow-green in color.
- Dry Cough: Some pneumonia patients, especially those caused by specific pathogens, may present with a persistent dry cough, meaning there is no mucus or very little mucus.
Shortness of Breath and Rapid Breathing
Due to the alveoli being filled with fluid, gas exchange is obstructed, leading patients to experience wheezing or difficulty breathing, particularly noticeable during activity or when speaking.
Chest Pain
Patients may experience sharp or pressing pain in the chest when taking deep breaths or coughing, medically referred to as pleuritic chest pain.
Cough with Sputum or Blood
Coughing may produce thick yellow or green sputum, and in severe cases, it may contain blood, requiring immediate consultation with a doctor.
Fever and Chills
Most patients will experience high fever accompanied by chills, shivering, or a sensation of coldness, which is a typical symptom of pneumonia.
Other Common Symptoms
These include fatigue, weakness, loss of appetite, nausea, or vomiting. Older adults are more likely to exhibit symptoms such as confusion or changes in mental status.
Risk Factors for Pneumonia
Certain populations are significantly at higher risk of contracting pneumonia:
Older Adults
Individuals aged 65 and above are at high risk for pneumonia due to weakened immune system function and often existing underlying health conditions.
People with Chronic Diseases
Those with chronic conditions like heart disease, diabetes, chronic obstructive pulmonary disease (COPD), asthma, or liver disease have a higher susceptibility to lung infections.
Immunocompromised Individuals
Patients undergoing cancer treatments or those requiring long-term use of steroids or immunosuppressive medications are also at an increased risk of infection.
Individuals with Unhealthy Lifestyle Habits
Smoking significantly damages lung defense mechanisms, greatly increasing the risk of lung infections. Chronic alcohol abuse can also impair immune function.
Delayed Treatment
Failure to receive appropriate treatment for common colds or flu in a timely manner, or neglecting early symptoms, can lead to secondary bacterial pneumonia.
When to Seek Medical Attention Immediately?
If you experience any of the following symptoms or signs of pneumonia, you should seek medical assistance immediately without delay:
- Severe difficulty or rapid breathing, with blue lips or fingertips.
- Persistent high fever (body temperature above 38.5°C) that does not improve with antipyretics.
- Intense chest pain, especially if it worsens with deep breathing.
- Confusion or altered consciousness, particularly in older adults.
- Coughing up blood or producing large amounts of thick mucus.
How is pneumonia diagnosed?
Accurate diagnosis of pneumonia is crucial for developing effective treatment plans. Doctors combine the patient's clinical symptoms, physical examination, and a series of laboratory and imaging tests to determine the nature, location, and severity of the lung infection.
An accurate diagnosis of pneumonia is crucial for formulating an effective treatment plan. Doctors will combine the patient's clinical symptoms, physical examination, and a range of laboratory and imaging tests to determine the nature, location, and severity of the lung infection.
Laboratory Tests
| Test | Purpose and Function |
| Sputum Culture Analysis | Analyzes the sputum produced from coughing to help identify specific bacteria or fungi causing lung infections for the development of a targeted antibiotic treatment plan. |
| Urine Antigen Test | Used for the rapid detection of specific bacterial pathogens, such as Streptococcus pneumoniae and Legionella pneumophila. |
| Complete Blood Count |
Assesses the level of the body's inflammatory response (e.g., changes in white blood cell count) and assists in determining whether the lung infection has spread to the bloodstream (i.e., bacteremia). |
Imaging Examinations
| Examination |
Purpose and Function |
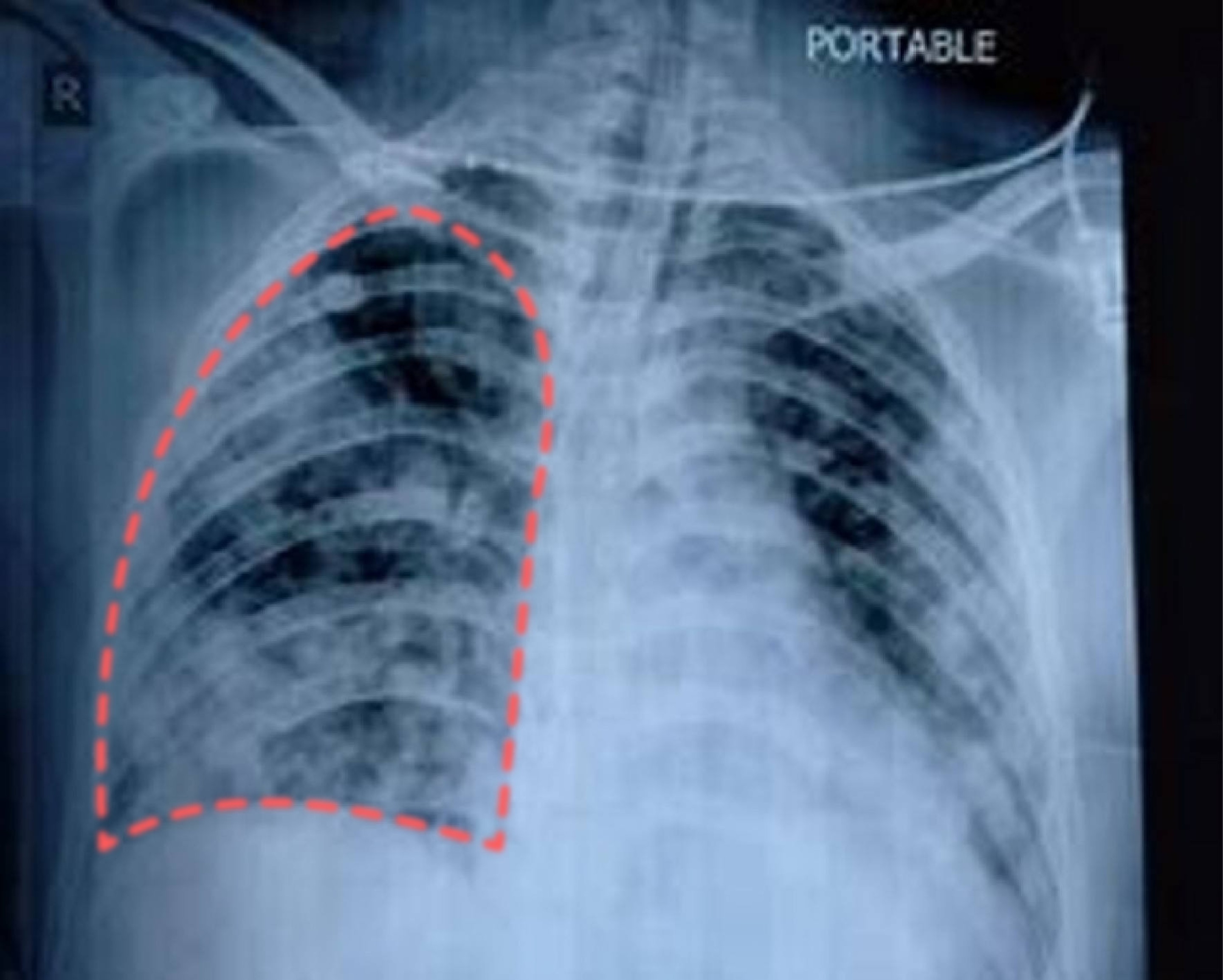
| Chest X-Ray Examination |
|
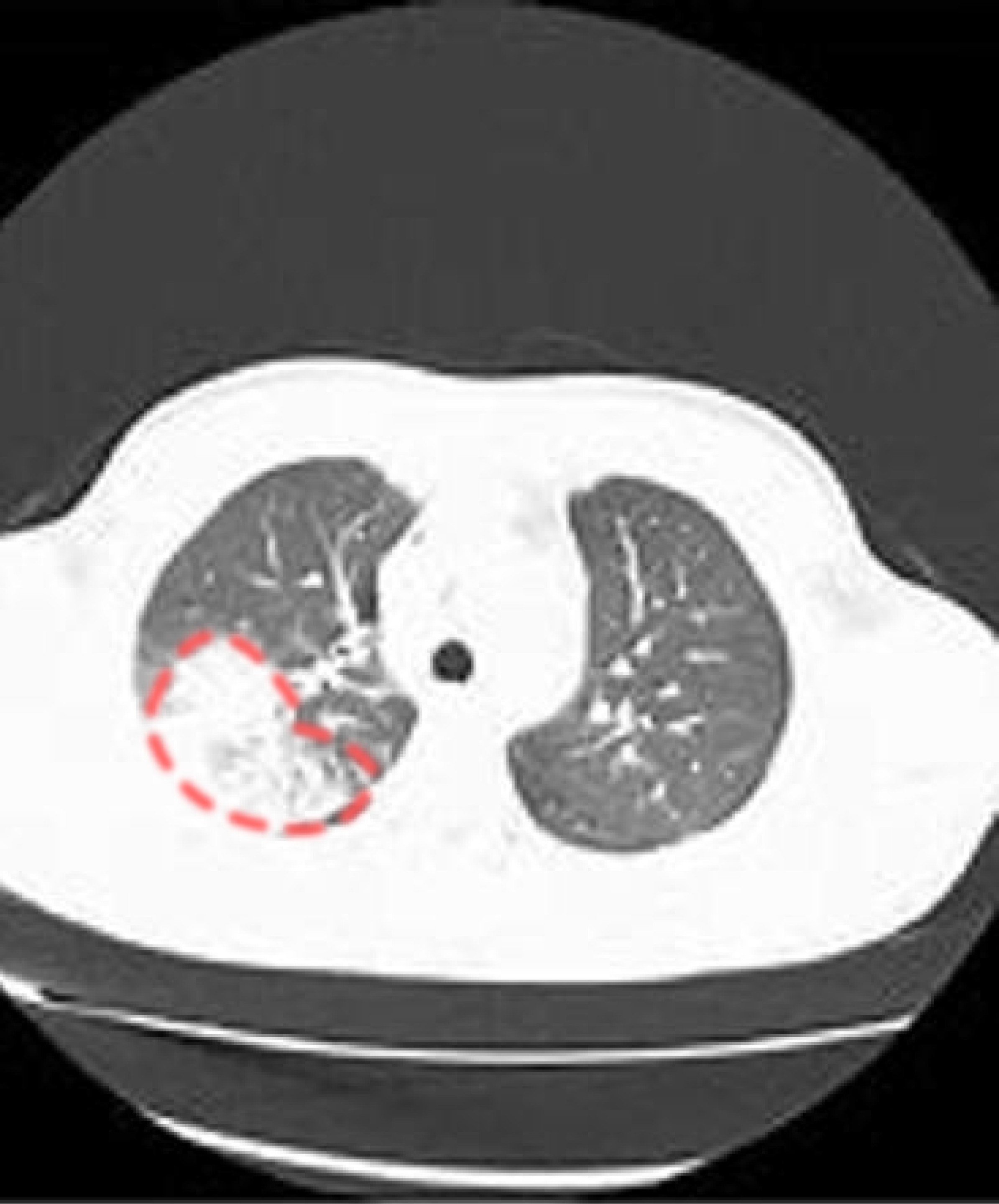
| Pulmonary Computed Tomography (CT) |
|
Invasive Examinations
| Examination |
Purpose and Function |
| Bronchoscopy | A flexible tube with a camera (bronchoscope) is inserted into the trachea and bronchi to directly observe the condition of the airways. This allows doctors to collect deep lung tissue or secretions for accurate pathogen analysis. (For details, refer to the Bronchoscopy Services at St. Paul's Hospital Endoscopy Center.) |
| Pleural Fluid Culture | For patients with pleural effusion (fluid accumulation between the lungs and chest wall). Doctors use a fine needle to withdraw the fluid for testing and culture to determine the nature of the fluid and the source of infection. |
If you suspect that you or a family member is experiencing symptoms related to pneumonia, it is recommended to seek consultation with a specialist in respiratory medicine as soon as possible. You can make an appointment for examination and diagnosis. through the St. Paul's Hospital Specialist Outpatient Department and arrange to see a doctor.
Treatment and Care for Pneumonia
The treatment plan for pneumonia depends on the cause, severity, and overall health status of the patient. Treatment is primarily divided into pathogen-targeted medication and supportive care to maintain bodily functions.
Medication Treatment
| Treatment Medication | Purpose and Function | Applicable Scope |
| Antibiotic Treatment | The core method for eliminating bacterial infections. Severe patients may require hospitalization for intravenous administration to ensure efficacy. | Bacterial pneumonia |
| Antiviral Medications | Inhibit viral replication and accelerate recovery. Common in pneumonia caused by influenza viruses. | Viral pneumonia |
| Corticosteroids | Help reduce pulmonary edema and inflammation. Generally used in cases of severe illness or excessive inflammatory response. | Severe inflammatory response |
| Expectorants and Bronchodilators | Expectorants thin thick mucus to aid in its expulsion; bronchodilators expand the bronchi to improve breathing difficulties. | Patients with excessive mucus, asthma, or chronic lung disease |
Supportive Treatment
In the treatment of pneumonia, supportive care is equally important as medication. It helps maintain vital signs, alleviate symptoms, and accelerate recovery.
| Treatment Item | Purpose and Function | Applicable Population |
| Oxygen Therapy | Provides additional medical oxygen through a nasal cannula or mask, ensuring vital organs receive sufficient oxygen to prevent tissue hypoxia. | Patients with significant respiratory difficulty or insufficient blood oxygen saturation |
| Hydration for Recovery | Dilutes mucus, making it easier to cough up and expel; also prevents dehydration caused by fever or rapid breathing. | All pneumonia patients |
| Chest Physiotherapy |
The Cardiopulmonary Rehabilitation Program aims to provide comprehensive physiotherapy assessment and treatment for patients with various respiratory conditions, including pneumonia. Individualized treatment plans are developed based on patient's condition, symptoms and needs, common treatment methods include: 1. Airway Clearance: Techniques such as percussion and vibration are used to help loosen and expel secretions accumulated in the lungs.
2. Exercise Training: Personalized exercise program is prescribed to improve lung function and overall fitness, facilitating return to daily living activities.
3. Functional Training: Gradual facilitation of everyday tasks, such as sitting out of bed and walking, to build stamina and confidence in returning to daily living activities.
4. Patient Education on Breathing Control: Teaching patients effective breathing techniques and strategies to help them better manage their condition. |
Patients with excessive mucus or difficulty expelling mucus |
| Nutritional Support | Provides adequate calories, protein, and vitamins to enhance body resistance, support the immune system in fighting infections, and promote recovery. | All patients, especially the elderly and those with chronic illnesses |
Possible Complications
If pneumonia is not treated in a timely manner or effectively controlled, the lung infection may spread and trigger a series of life-threatening severe complications.
| Complications | Definition and Impact to Patients |
| Respiratory Failure / Acute Respiratory Distress Syndrome (ARDS) | Severe lung damage that prevents sufficient oxygen from being effectively delivered to the blood. Patients may experience severe breathing difficulties and may require a ventilator to assist with respiration. |
| Bronchiectasis | Severe lung infection leads to permanent damage to the bronchial walls, causing abnormal dilation and relaxation of the airways, which affects the lungs' self-cleansing function and makes it easier to accumulate phlegm and infections repeatedly. |
| Pleural Effusion and Lung Abscess |
Pleural Effusion: Accumulation of fluid in the space between the lungs and the chest wall. Lung Abscess: Formation of a cavity filled with pus in lung tissue. Both conditions usually require drainage through medical procedures. |
| Septicemia and Bacteremia | The lung infection spreads to the bloodstream (bacteremia), leading to a life-threatening systemic inflammatory response, known as sepsis. |
| Multiple Organ Failure | Severe infections and sepsis can lead to the failure of multiple vital organs, including circulatory failure, kidney failure, and coagulation abnormalities. |
Methods for Preventing Pneumonia
Prevention is the most effective strategy for addressing pneumonia and reducing the risk of lung infections. We can approach this through active immunization, environmental protection, and lifestyle habits.
Vaccination Prevention (Active Immunization)
Receiving vaccines is a key step in preventing specific causes of pneumonia.
- Influenza Vaccine: Since influenza is a common viral cause of pneumonia, getting the flu vaccine each year is crucial, as it significantly reduces the risk of severe pneumonia following the flu.
- Pneumococcal Vaccine: Effective in preventing infections caused by pneumococci. It is strongly recommended for high-risk individuals, such as the elderly and those with chronic diseases.
Hygiene and Environmental Protection
Take proactive measures to prevent the spread of pathogens.
- Hand Washing: Maintaining good hand hygiene is the primary measure for preventing infection; thoroughly washing hands with soap and water is essential.
- Wearing Masks: It is recommended to wear masks in crowded places, poorly ventilated environments, or if experiencing respiratory symptoms.
- Avoiding Contact with Infected Individuals: Avoid close contact with people suffering from respiratory infections and ensure good indoor air circulation.
Healthy Lifestyle
Maintaining a balanced diet, regular exercise, and adequate sleep is fundamental to sustaining a robust immune system. Additionally, quitting smoking is particularly important for protecting lung health.
At-Risk Groups (Targeted Protection)
The elderly and those with weakened immune systems (including chronic disease patients) should pay special attention to keeping warm, avoiding high-risk areas, and undergoing regular health check-ups. They should receive appropriate vaccinations as advised by their doctors for targeted protection.
Common Questions About Pneumonia
Is pneumonia contagious?
Pathogens that cause pneumonia (such as bacteria or viruses) are typically spread through droplets, such as those produced by coughing or sneezing. However, the contagiousness varies depending on the cause of pneumonia.
Can pneumonia heal on its own?
While mild viral pneumonia may have some chance of self-resolution, in most cases, pneumonia is a serious lung infection. Without proper treatment—especially for bacterial pneumonia—it can rapidly worsen and become life-threatening. Diagnosis and the need for medication should be determined by a doctor.
Is atypical pneumonia the same as SARS?
The two should not be confused. Atypical pneumonia is a clinical category that refers to pneumonia caused by atypical pathogens (like Mycoplasma pneumoniae, Chlamydia, etc.), typically presenting with milder symptoms. In contrast, SARS (Severe Acute Respiratory Syndrome) is a specific, severe viral pneumonia caused by the SARS coronavirus.
How long does hospitalization for pneumonia typically last?
Hospitalization duration varies by individual. Mild pneumonia may not require hospitalization; home rest and medication per a doctor's instructions may suffice. Severe infections or high-risk patients (such as the elderly or those with chronic diseases) may require hospitalization for 3 to 4 days for intravenous antibiotics and supportive care.